Symptoms and Diagnosis for Parkinson’s
Everyone’s experience of Parkinson’s is different and therefore the condition does not affect everybody the same. The impact of Parkinson’s Disease can be unpredictable, and people will have good days and bad days. In saying that, there are some symptoms which are more common amongst people with Parkinson’s and it is likely that those who have the condition will experience one or more of the following:
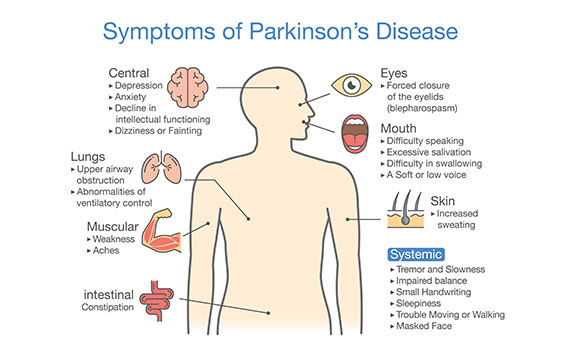
- Anxiety and Depression
- Fatigue
- Tremor (involuntary trembling or shaking movements)
- Constipation
- Muscle Rigidity (stiffness)
- Slowness of movement (bradykinesia)
- Balance problems (often leading to falls)
- Problems with posture (particularly a tendency to stoop forwards)
- Other possible symptoms include difficulty initiating movement (for example, when getting up from a chair)
- A shuffling gait when walking, and freezing when trying to move (especially in confined spaces such as doorways)
- Loss of Facial Expression/ Masked Face
Other possible symptoms include
- Problems with bladder control
- Loss of smell
- Speech problems (slow or slurred speech)
- Pain
- Memory problems
- Micrographia (Small Handwriting)
- Fine motor problems
- Problems opening and closing eyes
- Fainting
- Uncontrollable movement during sleep
Symptoms will also vary according to whether you have early onset Parkinson’s or are advanced with your condition. Early symptoms can be as subtle as having a loss of smell, constipation or changes in handwriting and therefore are often overlooked unless accompanied by additional symptoms. People with Advanced Parkinson’s are usually faced with more complexed symptoms which have more effect on day to day living. These may include, problems with swallowing, difficulty walking or standing up often requiring a wheelchair and assistance is likely to be needed in all areas of daily life.


Diagnosis
Diagnosing Parkinson’s Disease is not an easy or straightforward process as there is no specific test to conclude whether you have the condition. If you believe you have Parkinson’s, the first step would be to see your GP who will discuss your family history and symptoms. Your doctor may order lab tests, such as blood tests, to rule out other conditions that may be causing your symptoms.
In the early stages, it would be difficult for your GP to say whether you have Parkinson’s. It is likely that you would be referred to a specialist such as neurologist or geriactrician who would carry out some physical examinations and a neurological examination. Your neurologist may suggest a specific single-photon emission computerised tomography SPECT scan called a dopamine transporter (DAT) scan. Although this can help support the suspicion that you have Parkinson’s disease, it is your symptoms and neurologic examination that ultimately determine the correct diagnosis.
Most people do not require a DAT scan. In some cases, Imaging tests — such as MRI, CT, ultrasound of the brain, and PET scans — may also be used to help rule out other disorders. Imaging tests aren’t particularly helpful for diagnosing Parkinson’s disease.
A diagnosis of Parkinson’s disease is likely if you have at least 2 of the 3 following symptoms:
- shaking or tremor in a part of your body that usually only occurs at rest
- slowness of movement (bradykinesia)
- muscle stiffness (rigidity)
If you have recently been diagnosed with Parkinson’s, download our advice sheet here or email help@parkinsonscare.org.uk for more specific support.




